Stronger knees, smarter choices: rethinking osteoarthritis in women
It can start with a twinge that just gets worse. An aching, stiff knee when you get out of bed, grinding as you walk up and down the stairs. A sharp stab that shoots through your knee that stops you in your tracks as you squat down to get the washing out of the machine or squat down to reach for a drawer. There’s a loss of confidence as you as yourself: should I exercise on a sore, creaking knee? Will I do my knee long term harm if I keep running? How can I tell if it’s osteoarthritis?
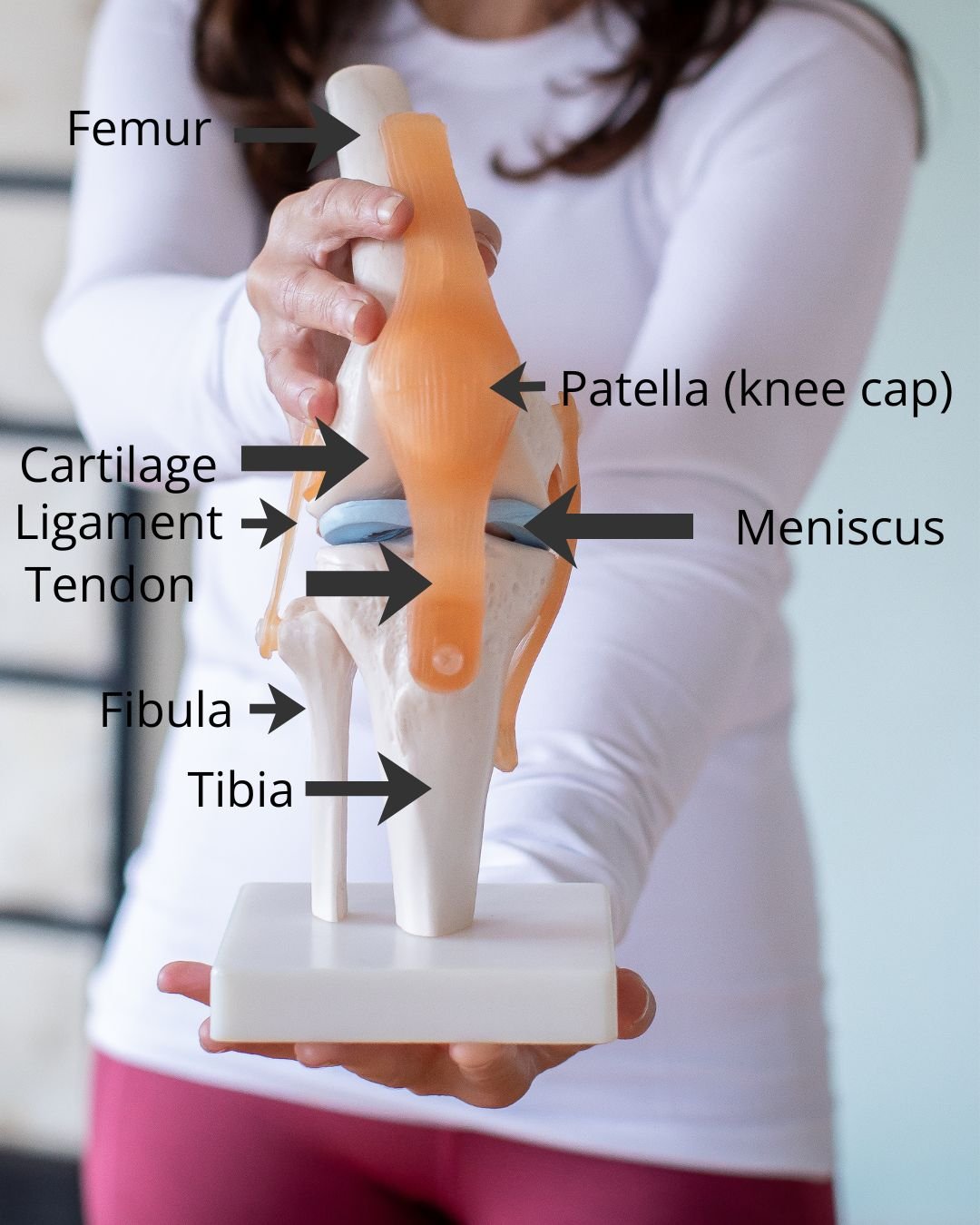
The knee joint is formed by the thigh bone (femur) and the shin bone (tibia) and the knee cap (patella) sits in a shallow groove at the front of the knee (see below) Osteoarthritis of the knee happens when the smooth cartilage at the end of the bones becomes thin and rough. Osteophytes - small bony growths - can develop on the joint surfaces. They don’t necessarily cause pain, but can do if the bony growth rubs against soft tissues or nerves or if they stop the joint gliding in its usual way. The knee also has cushioning cartilage called the meniscus (one on each side of the joint). The meniscus help absorb pressure across your knee. You can have osteoarthritis with or without meniscal problems, and problems with the meniscus make osteoarthritis more likely.
Women are up to 3 and a half times more likely than men to suffer from knee osteoarthritis, and the incidence increases significantly post menopause. It may be due to the changes in joint anatomy, alignment and strength, hormones and weight. Women are also much more likely to have an anterior cruciate ligament injury, which in turn dramatically increases the risk of osteoarthritis within 15 years.
How do you know if you have osteoarthritis or a meniscus problem?
If you’re unsure if you need a formal diagnosis via Xray (the gold standard), a Chartered Physio or Medic can guide you. They can also assess ligament or meniscal damage, as well as muscle weakness and flexibility. It’s a progressive condition, but with effective management you can minimise pain and stay as active as possible.
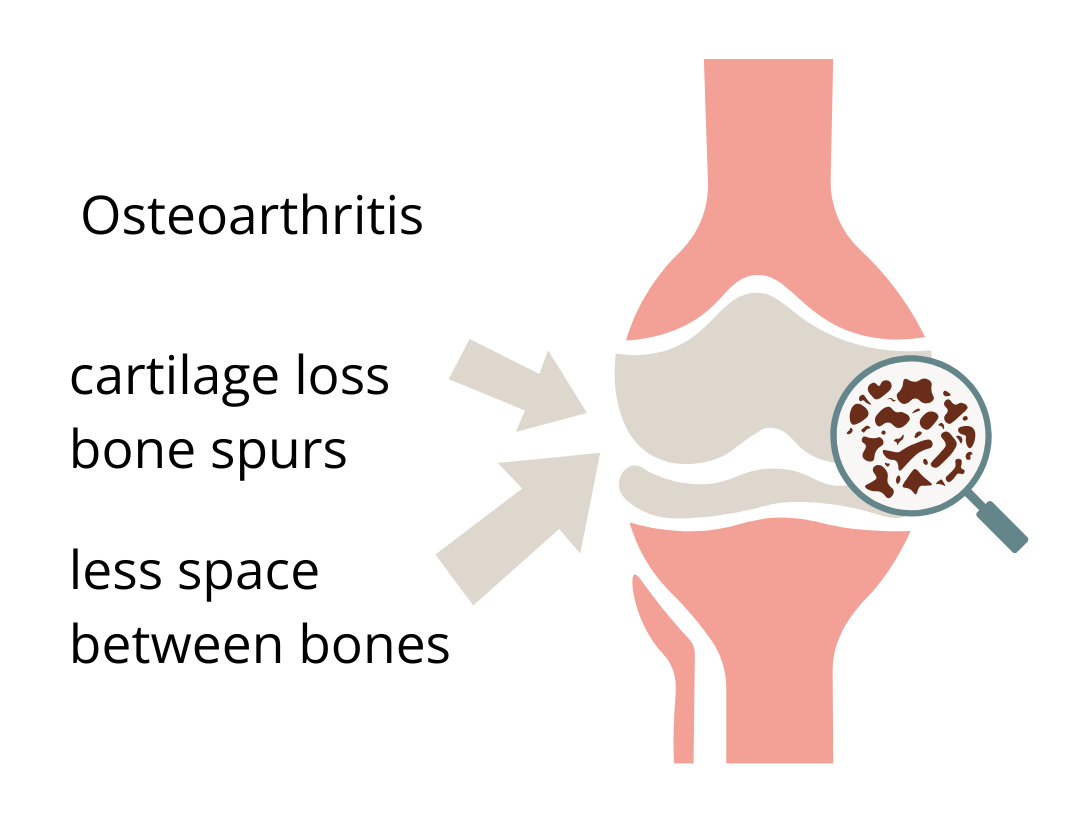
Here’s what an woman’s osteoarthritic knee looks like: Cartilage is lost at the ends of the bones, leaving less space between the joints. As cartilage wears down, bones can rub against each other. Bony spurs can also cause rubbing and there can be inflammation and swelling.
It’s a deceptive condition too. Severity on an xray doesn’t necessarily correlate with how you feel. One woman with severe arthritis might be able to run easily, another with only mild cartilage damage and early arthritis might find walking down stairs agonising. Understand your own unique situation - getting individualised advice is key.
Osteoarthritis - in need of a make over
Previously considered as a ‘wear and tear’ disorder, but it’s is more complex than just the grinding down of ageing bones. Wider inflammation, stress, depression, our nervous system and our pain perception all have a role to play in how it progresses and the pain we feel. Recent studies show that alongside getting older, low grade wider inflammation, carrying excess weight, metabolic problems like high blood pressure, high blood sugars, elevated cholesterol and even our gut microbiome can contribute to the progression of osteoarthritis.
On a positive note, taking positive lifestyle steps to improve mood and manage health can directly impact pain and long term outcomes.
Taking the pressure off joints by modifying activity and managing weight is essential, but not easy. Sometimes knee braces - specifically prescribed and fitted by a Physio, such as the Ossur braces, can help. That said, you do need to keep moving within what you can cope with. If you’re looking to do a walking holiday, walking poles can help you do the walks you want to do without overloading the leg joints.
How can I strengthen my knee if I have pain and osteoarthritis?
Strengthening around the knee joint, especially quads strength at the front of the joint and hamstring and calf strength at the back of the leg is vital in order to improve pain and minimise progression.
Is perimenopause making it worse?
Hormonal changes do impact joints and bones, but the effect is often indirect. You can get joint pain as a stand alone symptom of menopause,or the drop in oestrogen, alongside other factors, can compound your knee pain. If you want to discover more, join my Perimenopause and Joint Pain Masterclass this May.
Do weight loss injections help knee osteoarthritis?
A recent study (admittedly undertaken by the drug’s manufacturers) showed that semiglutide (Ozempic, Wegovy) improved osteoarthritic pain and symptoms in a predominantly female study group with an average age of 56 with an average BMI of 40.3. If you’re taking these drugs, or considering them, it’s vital to know how they work and how they affect bones and muscles.
Click below for female specific support to stay strong and nourished whilst using injections. This in turn helps them be more effective.
The knee - transferring forces from the spine and hips through to the foot. Problems above or below the joint can increase pressure on the knee, potentially making pain and swelling worse. Strengthening the muscles around the core and pelvis and having supportive footwear (support around the heel and under the arch of the foot) can help reduce this pressure and maintain better knee alignment.
Will running cause knee osteoarthritis or make it worse?
In short, no. Several studies show that there’s no connection between running and osteoarthritis.That said, these studies aren’t performed under perfect conditions, and runners may have a healthier lifestyle. We can’t say that for people that running won’t worsen knee osteoarthritis in people whose body mechanics, weight or genetics might predispose them to problems. If you find running makes your knee worse, seek Physio guidance. Exercise is an important part of managing arthritis, so if you find running or sports like tennis or padel make it worse, it might be worth doing less of it, mixing it with lower impact exercise that you enjoy, like cycling, swimming, pilates or golf or using a support to help you stay active.
The knee transmits forces from the pelvis and hip through to the foot and ankle. Keeping the core and hip muscles strong, maintaining balance and controlling the foot and ankle position with good footwear and strength will help the knee too.
If you plan to run, do prescribed sports specific knee exercises like modified lunges and single leg strength work.
Overall, a little movement, often, is really good for our joints: the more sedentary we are, the more joint problems, including osteoarthritis, we are likely to get.
References
Biddall, H et al. Once-Weekly Semaglutide in Persons with Obesity and Knee Osteoarthritis. New England Journal of Medicine. 2024;391:1573-1583. DOI: 10.1056/NEJMoa2403664
Kraus et al. An osteoarthritis pathophysiological continuum revealed by molecular biomarkers. Science Advances. 2024 Vol 10, Issue 17. DOI: 10.1126/sciadv.adj681
Mancino, F et al. Anterior cruciate ligament injuries in female athletes: risk factors and strategies for prevention. Bone Jt Open. 2024;5(2):94-100. doi:10.1302/2633-1462.52.BJO-2023-0166
Rodriguez-Merchan, E et al. Knee osteoarthritis following anterior cruciate ligament reconstruction: frequency, contributory elements and recent interventions to modify the route of degeneration. 2022 Nov;10(11):951–958. doi: 10.22038/ABJS.2021.52790.2616
Segal, A. et al. Sex differences in osteoarthritis prevalence, pain perception, physical function and therapeutics. Osteoarthritis and Cartilage 2024, 32 (9) 1045-1053. DOI:10.1016/j.joca.2024.04.002